Lateral release has been a controversial procedure for some time now. Lars Blønd gives his perspective on whether or not there is still a role for this procedure in a knee surgeon's armamentarium.
For what problem has lateral release been commonly performed in the past?
Lateral release was originally introduced by Ficat in 1975 for the 'hyperpressure syndrome' - a condition where the kneecap has for whatever reason become too tightly attached on the one side.
The symptom of hyperpressure is anterior knee pain, and typically the pain is aggravated by prolonged flexion, also called movie sign. It was hypothesized by Ficat that the lateral retinaculum was contracted and needed to be cut. Today the diagnosis of hyperpressure still exists and is recognized as one of many factors that may cause chronic anterior knee pain. The diagnosis is difficult to confirm by knee examination and by radiologic parameters. Tilt of the patella is often mentioned, but the tilt must be secondary to a tight lateral retinaculum and not secondary to trochlear dysplasia as it is in most circumstances.
Lateral release surgery became very popular during the eighties and nineties and was especially undertaken once keyhole surgery (arthroscopy) was introduced. Based on some initial reported good results, the indications expanded fast to also include patients with patellar instability. The logic at that time was that if the kneecap was unstable it was because the lateral retinaculum had pulled the patella out of its groove and therefore it had to be released. This surgery became very popular and frequently lateral release was combined with a tightening of the medial retinaculum, which is called medial reefing. The outcomes were reported as good, but today we know that these patients patellar stability declined after the first couple of years, and many needed new and more modern surgery.
[External hypertension syndrome of the patella. Its significance in the recognition of arthrosis][original article was in French] Ficat P, Ficat C and Bailleux A. Rev Chir Orthop Reparatrice Appar Mot. 1975 Jan-Feb;61(1):39-59.
Do you think lateral release has now developed a bad reputation?
Yes - Hughston back in 1988 reported on the negative outcome after lateral release and that some patients were going on to experience medial dislocations. In 2006 Christoforakis demonstrated in a biomechanical study that a lateral release made the kneecap even more laterally unstable. Since the late eighties most surgeons gradually omitted to perform lateral releases, and today the indications are limited and lateral release has got itself a bad reputation.
Medial subluxation of the patella as a complication of lateral retinacular release. Hughston JC and Deese M. Am J Sports Med. 1988 Jul-Aug;16(4):383-8.
Effects of lateral retinacular release on the lateral stability of the patella. Christoforakis J, Bull AM, Strachan RK, Shymkiw R, Senavongse W and Amis AA. Knee Surg Sports Traumatol Arthrosc. 2006 Mar;14(3):273-7. Epub 2005 Nov 26.
Is there a better procedure that has replaced lateral release?
After the disappointments of lateral release, the alternative procedure introduced by Slocum and his colleagues of Lateral Retinacular Lengthening (LRL) suddenly became more interesting. Then in 2012 a randomised trial from Pagenstert showed significant better result doing the lengthening compared to lateral release. Today I would say lateral retinacular lengthening has for most purposes replaced lateral release.
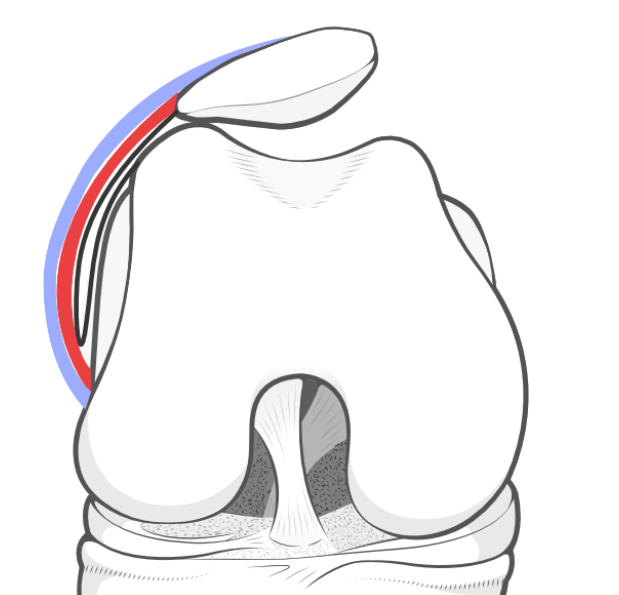 |
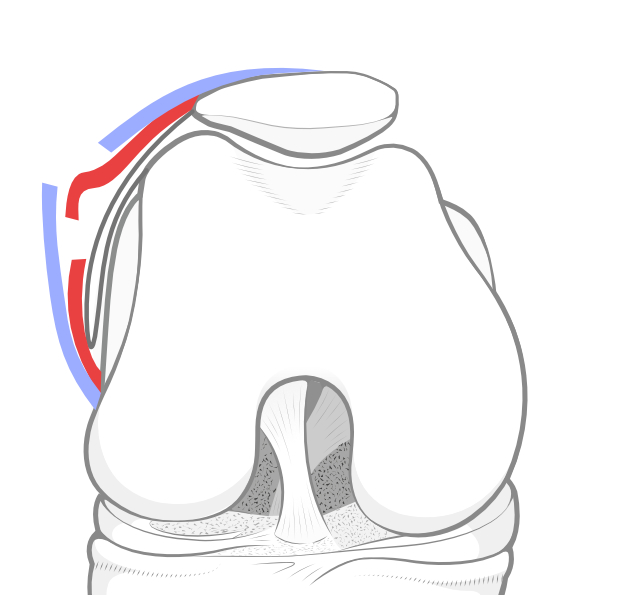 |
 |
| Tight lateral retinaculum causing patellar tilt and hyperpressure. | The independent release of the superficial and deep layers of the lateral retinaculum. | The lengthening of the retinaculum is carefully performed under control. |
Slocum DB, James SL, Larson RL. Surgical treatment of the dislocating patella in athletes. Presented at the Annual Meeting of the American Academy of Orthopaedic Surgeons. The Homestead, Hot Springs. 1973
Open lateral patellar retinacular lengthening versus open retinacular release in lateral patellar hypercompression syndrome: a prospective double-blinded comparative study on complications and outcome. Pagenstert G, Wolf N, Bachmann M, Gravius S, Barg A, Hintermann B, Wirtz DC, Valderrabano V and Leumann AG. Arthroscopy. 2012 Jun;28(6):788-97. doi: 10.1016/j.arthro.2011.11.004. Epub 2012 Feb 1.
In what specific circumstances do you yourself still perform lateral release?
I used to do many lateral releases but today I prefer lateral lengthening. I have not completely abandoned lateral release, but I only do arthroscopic lateral release in combination with arthroscopic trochleoplasty, and that is based on two things. The first is if the tissue is too swollen to do the lengthening. Also once a trochleoplasty has been done the patella is provided with significantly more bony stability and therefore the risk of creating a medial instability becomes only theoretical.
What can a surgeon do if a patient has worse instability after a previous lateral release?
Patients who suffer from medial instability consequent on an extensive lateral release can be severely troubled. Not only do they have the instability but usually they also suffer significant pain. Often these instabiities can be difficult for the surgeon to recognise. Many patients have been told that there is nothing wrong and nothing to do.
