Fifty years ago, Dr. Hughston, one of the founding fathers of American Sports Medicine, imparted a vernacular term for rotational deformities of the lower extremity – “Miserable Malalignment.”
Rotational deformities can frequently occur in childhood, evidenced by the appearance of their toes either pointed in (in-toeing) or out (out-toeing), and if caused as a part of normal development generally corrects itself once the child is weight bearing – without long lasting impact to the musculoskeletal system.
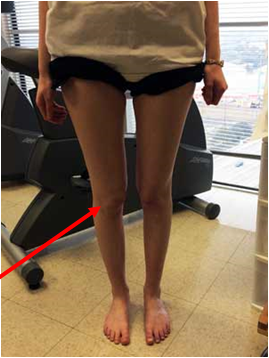
If the deformity is caused by another problem, it may persist into adulthood and become increasingly more difficult to identify. In the photograph to the right, one can recognize how the knees are turned inward, while the feet turn forward.

To the untrained eye, the subtle signs of Rotational Deformity may go undetected. Notice how the feet are rotated outward, on the left demonstrating pathological external tibial torsion. On the right, the tibias, representing a “pointer” for the femurs rotate internally in an excessive manner. (Not externally, because the knees are flexed to 90 degrees. This is confusing even for a clinician).
 The rotational component of combined deformities can be diagnosed by a careful physical examination, quantified and confirmed by a specially done CT or MRI scan.
The rotational component of combined deformities can be diagnosed by a careful physical examination, quantified and confirmed by a specially done CT or MRI scan.
Photo right: Childhood photo of patient showing visible malrotation.
The rotation comes from a rotation of either the femur (upper leg bone) or the tibia (lower leg bone). The deformity generally affects both legs and can often be a combination of angular and rotational components.
Treating Rotational Deformity
There are both surgical and nonsurgical treatments for rotational deformity. The right treatment for each patient will depend on the type and severity of their deformity, as well as previous treatments they may have undergone.
This condition is frequently misdiagnosed and can cause pain for years before a physician trained to identify the signs is able to correct the problem.
Treating rotational deformity generally entails the use of several different osteotomy procedures. Osteotomy means bone cutting and entails a transverse bone cut just above or below a joint, shifting the malrotated lower limb segment to the known anatomic alignment, with immediate repair of the bone using a stable plate and screw construct. Since the cut is transverse, no bone is either added or removed, and the fixation is stable – accelerated rehabilitation is instituted.
The collective goal of these osteotomy procedures is to restore proper alignment to the lower limb, preventing degeneration (progressing to osteoarthritis), as well as correct the abnormality and establish anatomical correctness – restoring optimal leg function for patients wanting to return to an athletic or active lifestyle.
Each osteotomy procedure is designed to accomplish a different goal and are selected based on the anatomy of the deformity and other specific circumstances - to repair an individual deformity.:
- Femoral Osteotomy, either nearer to the hip, or to the knee typically used to repair an internal rotation deformity, commonly called anteversion or antetorsion that is greater than 30 degrees.
- Proximal Tibial Osteotomy typically used to repair an external rotation deformity that is between 35 and 45 degrees.
- Distal tibial and fibular osteotomy: commonly used to repair an external rotation deformity that is equal or greater than 40 degrees.
- Osteotomy of the Tibial Tubercle: is occasionally necessary to repair a patella mechanism that causes the patella to ride to high (patella alta) and not engage its groove on the femur or redirect a tibial tubercle that is positioned too far laterally or medially.
Derotational Proximal Femoral Osteotomy
 A derotational proximal femoral osteotomy focuses on the realignment of the femur for purposes of obtaining anatomic alignment of the limb below the osteotomy, inclusive of the patella, leg, ankle, and foot. Typically, it will place the femoral groove (that articulates with the patella) directly under the patella.
A derotational proximal femoral osteotomy focuses on the realignment of the femur for purposes of obtaining anatomic alignment of the limb below the osteotomy, inclusive of the patella, leg, ankle, and foot. Typically, it will place the femoral groove (that articulates with the patella) directly under the patella.
Photo right: Postoperative correction of rotational deformity.
A proximal femoral osteotomy is most commonly performed on younger people whose complaints are that of a deformity, and associated lower extremity problems inclusive of patella femoral pain and recurrent subluxation or dislocations. In these patients CT or MRI imaging will reveal antetorsion of 30 degrees or greater. A transverse cut made just below the hip is made and the rotation is reduced to 15 degrees with is the normal amount of antetorsion.
Proximal and Distal Tibial Osteotomy
The Proximal Tibial Osteotomy has also proven to be a safe and effective procedure. A proximal tibial osteotomy is most commonly performed on younger people whose complaints are that of a deformity and have associated lower extremity problems inclusive of patella femoral pain and recurrent subluxation or dislocations. In these patients CT or MRI imaging will reveal excessive external rotation of between 35 and 40 degrees. A transverse cut made just below the knee is made and the rotation is reduced to 23 degrees, which is the normal amount of external rotation.
A pre-contoured, low profile plate and screws are inserted to keep the osteotomy in place such that immediate rehabilitation can proceed – emphasizing knee range of motion and weight bearing.
The amount of correction possible with the proximal osteotomy is limited by the presence of the common peroneal nerve, which winds around the neck of the fibula. Rotation of the tibial osteotomy in excess of 20 degrees will cause stretching and dysfunction of this important nerve. Accordingly, when corrections of greater than 20 degrees are necessary, the osteotomy is performed nearer to the ankle, distal to where the motor branches from the peroneal nerve have already supplied their muscles.
Osteotomy of the Tibial Tubercle
An osteotomy of the tibial tubercle is a surgical procedure performed along with other procedures to treat patellar instability and patellofemoral pain, when the patella either rides too high or is inserted too lateral on the proximal tibia. A tibial tubercle transfer technique involves the realignment of the tibial tubercle (bump at the front of the shin bone) allowing the knee cap (patella) to traverse the center of the femoral groove. The patellar tracking is corrected by moving the tibial tubercle distally and/or medially, towards the inside portion of the leg. This removes the load from the painful portions of the knee cap.
A key component of this, as with any procedure, is established long before the patient arrives in the operating room. It is the thought process and plan that the patient and orthopaedic surgeon work up together, known as preoperative planning.
The orthopaedic surgeon first considers the complex deformities before proceeding with the procedure. After careful consideration, quantitative imaging (MRI or CT scan) including the hip, knee and ankle is performed so that measurements of rotation are accurately made.
Indications for repair include patients who are unable to live the life they want because of limb pain, instability, or deformity – and whose objective measurements fall far outside of the normal bell distribution. Surgery for correction is performed on all deformed bones at the same time, replacing the deformity with anatomic rotations that are at the 50% mark of normal range.
Although the risks associated with these osteotomy procedures are low, the most common complications include:
- Infection
- Blood clots
- Stiffness of the knee joint
- Injuries to vessels and nerves
- Failure of the osteotomy to heal
Further reading
View postoperative results from a left-leg rotational deformity repair.