This article discusses the surgery for a patient with unresolved painful late Osgood Schlatter's disease.
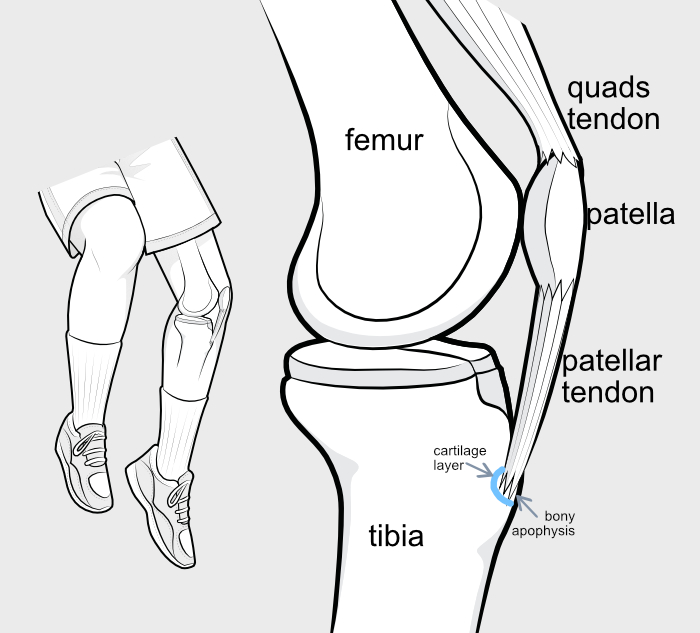
In children who are not yet fully grown the bone of the bump and the big tibia bone itself are not one solid unit, but there is a softer cartilage interface between the bump and the main bone. The little bit where the tendon attaches is called the 'apophysis'.
The cartilage layer allows for bone growth in the growing child, but when the child reaches maturity this layer, too, transforms into bone and the apophysis becomes a true part of the main bone. Children with Osgood Schlatters have what is called 'traction apophysis' - jumping too much causes the tendon to pull excessively on the apophysis, and the region becomes inflamed. Their doctors generally advise them to reduce their sporting activities until they reach bony maturity to allow the natural fusion to safely occur.
Unresolved Osgood Schlatter's Disease
Sometimes, however, the period and extent of the traction may have been too great, and even after skeletal maturity some of the apophysis may fail to fuse to the main tibia bone, and remain separated as a small 'ossicle' localised within the patella tendon together with a little bump remaining on the tibia. The friction between these can cause inflammation and pain.
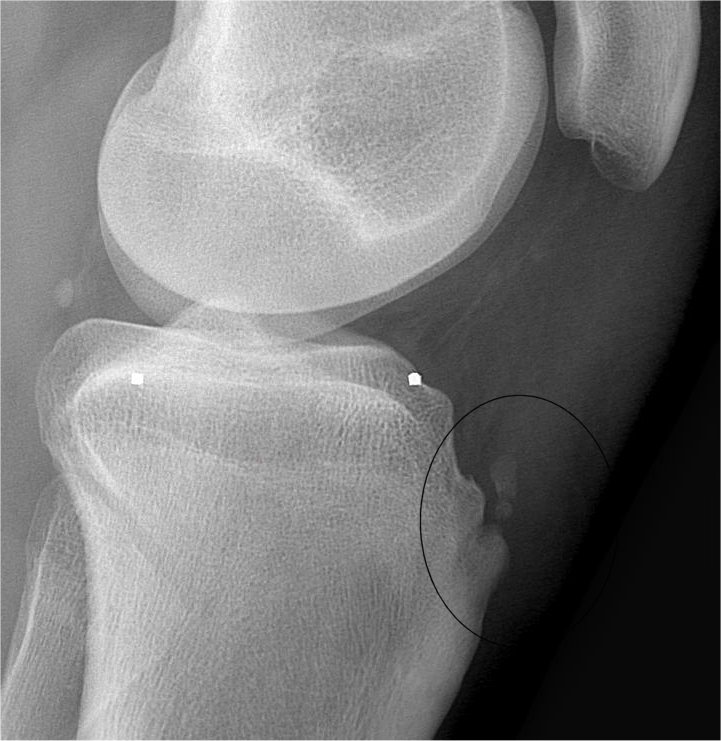
If you look at the X-ray now - at the area circled in black - you will be able to appreciate that there is some distortion of the main bone in the tubercle region, and you will also see the completely separate 'ossicle'. We know that the person has reached skeletal maturity because there is no longer any growth plate visible on the two long bones - these have already fused and become bone.
A young person who suffered from Osgood Schlatters as a child may be disappointed to find that his symptoms of pain over the tubercle area continue into adulthood and the bump in this area may continue to be prominent and tender. Typically the patient complains of pain in the tubercle area when lying on the affected knee or with strenuous activity.
When they come at this stage to the surgeon they may be offered a conservative regime, with anti-inflammatory medication and local steroid into the bursa behind the tendon. If this does not resolve the symptoms, sonography can be helpful.
Bursoscopic excision of Ossicle
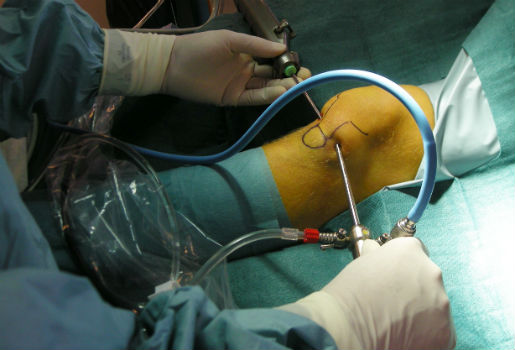
Initially portals (keyholes) are made on both sides of the patellar tendon a little proximal to (higher up from) the tibial tubercle. On one side I introduce an arthroscope, which has a light source, camera and fluid irrigation, and on the other side I introduce a motorised instrument which has a rotating shaver burr at its end.
Both of these instruments are passed into a natural space - or bursa - that exists under the tendon I burr away (debride) the excess prominent bone on the tibia, starting proximally and then continue distally (from top to bottom) until the patellar attachment is reached.

Then I turn my attention to the ossicle itself. I use a probe and then I shave it free from the softer tissues encasing it, and then I use a grasper to take it out. You can see the ossicle sandwiched between the ends of the grasper. It looks quite big but the camera magnifies it, and also there is soft tissue surrounding it.
Removal of the ossicle usually resolves the patient's pain.
Further Reading
https://www.ncbi.nlm.nih.gov/pubmed/?term=eun+osgood
http://emedicine.medscape.com/article/1993268-overview
https://radiopaedia.org/articles/osgood-schlatter-disease
http://drrobertlaprademd.com/wp-content/uploads/2015/07/anatomy-of-the-d...
