X-rays should reveal any bony damage to the knee, but often soft tissue damage can be inferred from the bony information.
 First published by knee surgeon Adrian Wilson in 2010, and reviewed August 2023 by Dr Sheila Strover (Clinical Editor)
First published by knee surgeon Adrian Wilson in 2010, and reviewed August 2023 by Dr Sheila Strover (Clinical Editor)
X-rays after an acute knee injury
Moving on from the clinical examination everyone that has this type of injury – and this is especially relevant in children – they all need to have X-rays to look for a bony injury.
The main thing X-ray will pick up is a fracture, but it will also pick up subtle abnormalities – say if you have got a major ligament problem you will see an increased space on the side where the ligament is ruptured – the gap will be too big and it won’t be symmetrical with the other side as it should be.
There are certain other things that the X-ray will pick up, such as –
- whether there is blood in the knee as you will see what we call a ‘lipohaemarthrosis’ or evidence of an effusion or swelling, and often you can see the fat on the X-ray
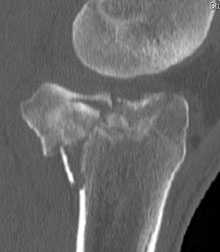
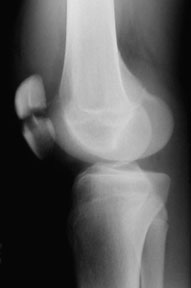 any obvious breaks, and the things we are looking for here include patellar fracture (X-ray on left shows the patella broken in two), tibial plateau fracture (X-ray on the right shows the tibial plateau shattered into bits), osteochondral injury (small flake of bone knocked off) or perhaps even a Hoffa’s fracture which is an eponymous name which is used for a fracture which occurs at the back of the femur where part of the articular surface (joint surface) and bone break free.
any obvious breaks, and the things we are looking for here include patellar fracture (X-ray on left shows the patella broken in two), tibial plateau fracture (X-ray on the right shows the tibial plateau shattered into bits), osteochondral injury (small flake of bone knocked off) or perhaps even a Hoffa’s fracture which is an eponymous name which is used for a fracture which occurs at the back of the femur where part of the articular surface (joint surface) and bone break free.
- a Segond fracture which is pathognomonic (definitive evidence) of an ACL rupture, and that is a tiny little flake of bone that comes off usually on the lateral side (although it can occur on the medial side). It indicates that the knee has been torn in such a way that the ACL must have been ruptured for that to occur.
- In the paediatric group we are looking for ‘tibial spine pulloff’. Most children who have a twisting injury don’t tend to rupture the ligament (ACL) but tend instead to pull the bony attachment off and the ligament tends to remain intact and that is very easily seen on X-ray unless they are very young, so we look closely in a child to see if there has been a pulloff of the anterior tibial spine because that is a surgical emergency.
Plateau fractures and fractures in general are thus picked up by the X-rays but you do need to get a full series of four X-rays – an AP view, a lateral view, a skyline view, a Rosenberg or Schluss view which is the tunnel view and which shows the osteochondral injury. Someone senior needs to look at the X-rays as the signs may be subtle and easily missed.
