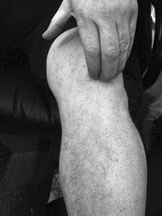
- The patella - important anatomical relationships
-
Pain syndromes related to the patella
- The unstable patella
- Cartilage damage of the patella
- Fractures and tendon ruptures involving the patellar mechanism
When pain is experienced around the patella the actual cause may often be difficult to diagnose. Certain groups of symptoms have earned the name of syndrome as the particular symptoms tend to be associated with one another.
Pain in the front of the knee
Pain in the front of the knee is often referred to loosely as anterior knee pain syndrome or patellofemoral syndrome, but these are non-specific descriptions and are not diagnoses in their own right.
A syndrome is a set of symptoms that tend to occur together - rather than being an actual diagnosis of the cause of the symptoms. Some patients may have a collection of symptoms predominated by pain which may be vague in nature and is experienced behind or around the front of the kneecap. Together with this pain, patients may complain that there is discomfort on descending or ascending stairs, or walking downhill or on uneven surfaces. The knee may become stiff and uncomfortable after sitting for a long time. There may be crunchy noises or a grating sensation (patellar crepitus) on bending and straightening the knees.
The strain on the patella may be the result of an abnormality anywhere in the chain of structures influencing the alignment or tracking of the patella - from the hip, through the femur bone, the tibia bone and down to the feet - and including the quadriceps muscle (of which a part, the rectus femoris, is shown in the illustration below) and its attachment to the tibial tubercle.
Hip imbalance
Pain at the front of the knee may arise from imbalance in the hip adductors and abductors, or weakness of the hip external rotators.
Tight iliotibial band (ITB)
Another cause of pain at the front of the knee may be tightness of the iliotibial band, the fibrous band that runs the full length of the upper leg from hip to knee.
Quads weakness
Weak quadriceps muscles, especially the oblique part of the vastus medialis head known as the VMO (vastus medialis obliquus), may allow the patella to pull to the lateral side. The VMO plays a big role in tightening the medial retinaculum and keeping the patella aligned in the centre of the underlying groove.
Quads/hamstrings imbalance
It has been found in patients with pain in the front of the knee that the hamstrings are often weak in relation to the quadriceps muscle. A balance in quads and hams contributes to patellar stability.
Abnormalities of the arch of the foot
Arch abnormalities, especially flat-footedness, can cause an alteration in the alignment of the whole limb with malalignment and maltracking of the kneecap.
Tight calf muscles
Tight calf muscles can cause a compensatory rolling-in of the foot, with consequent alteration of limb alignment and stress on the kneecap.
Referred pain
Conditions of the hip and lower back may cause the patient to experience pain in the front of the knee. This is called referred pain and is a key reason why examination of the knee should always be accompanied by examination of the hip.
Overuse disorders involving the patella
Patellar tendinosis
Patellar tendinosis, or jumper's knee, is a painful condition of the tendon below the kneecap, usually involving degeneration of the tendon substance.
It is a disabling condition which frequently affects sportspeople:
- mainly jumping sports
- insidious onset of pain localised to the area just under the kneecap
- painful when walking or running up slopes, or getting up from sitting
- tender to deep pressure underneath the kneecap
Pre-patellar bursitis
Pre-patellar bursitis or housemaid's knee is due to inflammation of the bursa (lubricating pocket) in front of the patella.
Traction apophysitis
When the attachment of the patellar tendon to the bone becomes strained
- Osgood Schlatter's disease - traction apophysitis at the attachment of the tendon to the tibial tubercle
- Sinding-Larsen & Johannsen Disease - traction apophysitis at the attachment of the tendon to the undersurface of the patella
Quadriceps tendinosis
Painful degeneration of the inside of the quadriceps tendon above the kneecap
Patellofemoral arthritis
Arthritic cartilage breakdown can affect either or both of the joint surfaces in the patellofemoral joint - that is, the underside of the patella or the groove of the trochlea. Options for management include cartilage repair procedures, patellofemoral resurfacing, or total knee replacement.
Neuroma
A neuroma is a benign overgrowth of nerves, often in response to trauma or surgery. In the knee the commonest site is in the anteromedial part of the knee related to the infrapatellar branch of the saphenous nerve. The small tumour-like overgrowth is sensitive to pressure and pain is relieved when injected with local anaesthetic solution as a diagnostic test.
Nonspecific Chronic Anteromedial Knee Pain Neuroma as a Cause of Infrapatellar Pain Syndrome: Case Study and Literature Review. Grabowski R, Gobbi A, Zabierek S and Domzalski ME. Orthop J Sports Med. 2018 Jan; 6(1): 2325967117751042.
Fat pad syndrome

There are three main fat pads in the knee, but the most important is the one underneath the patellar tendon - the infrapatellar or Hoffa's fat pad. The fat pads are normal structures that act as shock absorbers, but also have a function in healing.
The term fat pad syndrome relates rather vaguely to pain experienced in the front of the knee and which is thought to originate from problems within the fat pad.
Fat pad disorders
Abnormalities of the fat pad are most commonly a result of direct injury, of which arthroscopy is the most frequent cause! Other causes of trauma include posterior and superior impingements - where the fat pad is too big it can get caught in the joint at the top (superior) or at the back of it (posterior). The fat pad can also be damaged during patellar dislocation. Trauma to the fat pad can also damage the infrapatellar plica that is a normal anatomical structure posterior to the fat pad. Within the fat pad one also may have inflammatory disorders and synovial and chondral tumours (growths) (arising from joint-lining cells and cartilage cells). These tumours can sometimes be nasty. One can get cysts in the fat pad (fluid filled pockets). No-one really knows the cause of this, but they can sometimes be confused with a cyst of the meniscus or cruciate ligament. The posterior border of the fat pad may also become inflamed and may cause increased joint fluid (effusion).
Hoffa's disease
Hoffa's disease specifically relates to impingement of a hypertrophic (over-sized) fat pad in a normal joint between the joint surfaces of the knee (between femur and patella or between tibia and patella) leading to swelling or oedema of the fat pad and fibrosis within the fat pad.
The characteristic symptom of Hoffa's disease is chronic ('going on for a long time') anterior knee pain mostly under the patella. It is more of a discomfort than a sharp pain. The knee may feel weak and sometimes swell. If the knee has been damaged in an injury with Hoffa's pad rupture-detachment then the pain may be acute ('coming on suddenly), the functional impairment may mimic a ligament injury, and the knee may be very swollen with blood in the joint fluid.
In testing for Hoffa's disease, one tries to elicit a 'Hoffa's sign' which is highly specific. The examiner applies pressure to the margins of the patellar tendon when the knee is bent, and maintains the pressure while the knee is straightened. In a positive result this causes a sudden severe pain and the patient refuses to keep on straightening the leg. MRI is good for showing the fat pad, unlike arthroscopy where it cannot be clearly seen because it is usually behind the light source and instruments.
An injection of local anaesthetic and steroid into the fat pad itself helps to decide if the fat pad is implicated in the pain that the the patient is experiencing. If it is then it will cause a transient relief of symptoms. Fat pad pathology is usually secondary to other knee joint problems, and its primary involvement is rare.
Hoffa's syndrome
Hoffa's syndrome is similar but the symptoms occur in conjunction with concomitant pathology.
Infrapatellar fat pad syndrome : a review of anatomy, function, treatment and dynamics. Mace J, Bhatti W, Anand S. Acta Orthop. Belg., 2016, 82, 94-101.
---
Kneecap pain is often enigmatic, that is it comes and goes or may be experienced in different places at different times.
Although Patellofemoral Syndrome is commonly flagged as the cause of a patient's pain experienced around the kneecap, patellofemoral syndrome itself is not a discrete condition, but rather a group of symptoms related to the alignment or tracking of the kneecap but which may have a variety of contributing causes. These causes may be related, for example a flat foot may also contribute to stress on the lower back, and both of these may lead to pain around the kneecap via different routes. Symptoms may vary depending on muscle fitness, muscle balance (eg quadriceps/hamstrings balance), footware, insoles, cycle saddle height, alterations in gait, unusual levels of exercise, or combinations of such factors.
Plicae may be unrecognised as a cause of symptoms
Plicae are normal folds of joint lining, and they vary from person to person. Some people have no plicae at all and other may have plical folds stretching right across the joint space. The problem with surgeons being vague about plicae is that the medical literature has in the past stressed that plicae are normal and do not cause pain, while many other authors have convincingly demonstrated certain thickened plica as causing joint surface damage. Plicae may go unreported on MRI scan, even though they may be visible, as the radiologist may be one of those clinicians who consider them to be unimportant.
Referred pain may complicate the picture
Referred pain is pain experienced in one place but which is actually being triggered in another.It is important that the investigating clinician keeps in mind that pain experienced in the knee may in fact be arising elsewhere.
Trigger point pain
Trigger points are 'knots' in the muscles that may cause tenderness at discrete points around the knee, but they also may trigger pain which appears to come from the knee itself. To add to the difficulty knee problems may cause trigger points to flare up.
Pain referred from the hip
Children may be born with hip problems, for example Perthes Disease, and complain only of knee pain. Adolescents with Slipped Capital Epiphysis of the hip may experience pain in the knee. Adults with hip arthritis may experience severe knee pain.
A hip examination should be a normal part of any investigation of knee pain. It is a curious fact that a hip problem may present with only the symptom of pain experienced in the knee. In this case the knee may be blamed although it may be completely normal.
Pain referred from the lower spine
A low back problem, such as a herniated disc, may lead to pain in the knee, and also pain in other parts of the lower leg. Usually the pain is experienced in a specific distribution depending on the which vertebral disc is damaged.
Complex regional pain syndrome
Previously called RSD (reflex sympathetic dystrophy) is another form of referred pain. This is a condition where the knee has suffered an insult - injury or surgery - and the pain, instead of getting better, becomes unremitting and out of proportion to the apparent situation. The patient may also feel funny feelings in the region, and the skin may become discoloured and blotchy and exquisitely sensitive to even the slightest touch.
This diagnosis is often missed in the early stages - but it is important to be aware of it as it may respond to early treatment, but if allowed to progress the limb may become permanently wasted.
Inconsistent terminology may lead to confusion
Different clinicians may use different words when describing the same problem. There is no clear standardisation of patellar terminology. So this makes the interpretation of medical publications frequently confusing as authors and readers may have different ideas of what is being described.
Plica syndrome
The 'plica syndrome' is a group of symptoms that are commonly associated with the presence of an abnormally thickened plica.
A plica is a fold of the soft inner lining of the knee joint (this lining is called the 'synovium', so a plica is also often called a 'synovial plica').
Plicae (plural) are remnants of structures which existed in the foetus (in the womb) and which subsequently fell away to a lesser or greater extent as the knee developed. In some people they are still significant stuctures and in other people they may be completely absent.
A plica may become symptomatic when it is nipped between structures in the knee, becoming inflamed and eventually thickened.
Symptoms of an abnormal plica
Where plicae are situated
Typically plicae are found in three positions -
- suprapatellar (SPP) (above the patella or kneecap)
- infrapatellar (IPP) (below the patella), sometimes called the 'ligamentum mucosum' or 'filmy ligament' as it mimics the cruciate ligament inside the knee, but is not a ligament at all.
- medial (MPP) (on the inner aspect of the knee). It may form a shelf-like band and is then referred to as a 'medial shelf'.
| In this illustration, looking at the knee bones of the right knee from its inner aspect, you can see the relationship of the media and suprapatellar plica. Here the leg is straight. | 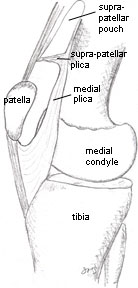 |
| When the knee is bent, the plicae taughten, and a medial plica can snap abruptly over the medial femoral condyle, while the suprapatellar plica may be nipped between condyle and the quadriceps tendon. |  |
| The medial plica can also become nipped between patella and condyle, causing momentary pain and 'giving way'. | 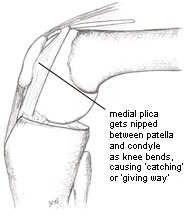 |
| Photo taken during arthroscopy to show a plica being nipped. | 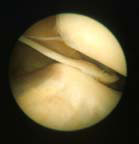 |
| The region marked in this illustration is often tender, and careful examination may reveal a chord-like thickening. |  |
PREVIOUS PART: The patella - important anatomical relationships
NEXT PART: The unstable patella