- The patella - important anatomical relationships
- Pain syndromes related to the patella
- The unstable patella
- Cartilage damage of the patella
-
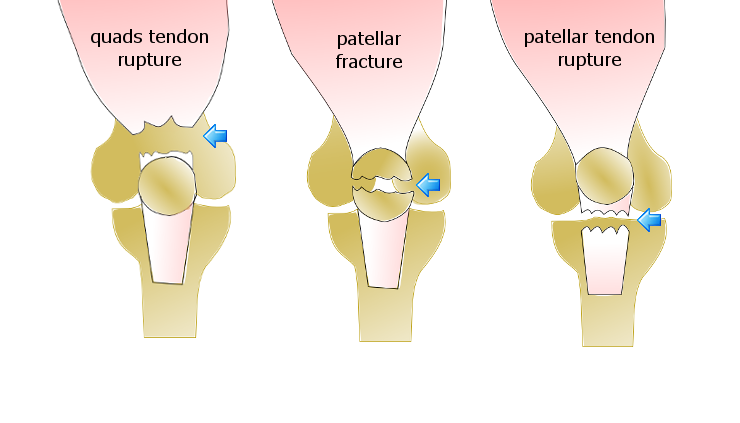
Fractures and tendon ruptures involving the patellar mechanism

The extensor mechanism includes -
- the quadriceps ('quads') muscle group that reaches from hip and upper femur to the knee, with the four muscles in the group joining together at the bottom to form the quads tendon
- the quads tendon itself
- the patella, which is actually housed within the quads tendon
- the patellar tendon, below the patella and which is in reality a ligament rather than a tendon, as it reaches from bone to bone (rather than muscle to bone)
Contraction of the quads muscles thus puts tension on this entire complex to pull the leg straight, and the patella acts to increase the leverage of the whole. During extension, the patella and the two tendons are subjected to high tensile forces, and the patella is also subjected to high compressive forces where it makes contact with the femur bone.
Failure of the extensor mechanism
Main differences between rupture of an extensor tendon and patellar fracture
Although a patellar fracture may occur at any age, a quads tendon rupture usually occurs in patients over 40 years of age and a patellar tendon rupture in sporting patients under 40 years of age.
Patellar fracture
In terms of the main differences, the big factor with a patellar fracture is that the joint surface is often disrupted, and the joint cartilage damaged. With the other two types of rupture, the challenge is to secure the soft tissue back onto the bone without there being any re-rupture.
Quads tendon rupture
In quads tendon rupture the bulk of the muscle may recoil with a large gap above the patella. This may be missed because these injuries are often associated with tremendous localised swelling. In patellar tendon rupture, the patella is pulled up into an abnormally high position from which it must be retrieved and the anatomy restored as soon as possible.
Patellar tendon rupture
Causes of patellar tendon rupture include:
- direct blow or cut to the tendon
- stress combined with pre-existing weakness in the tendon (possibly from one of - steroid injection into the area, gout, repetitive exercise strain, arthritis, diabetes, growths)
Symptoms include difficulty straightening the knee against gravity compared to the other side, and a tender, painful gap below the kneecap. X-ray may show patella alta (high riding kneecap).
The patient is usually under 40 years of age. Above that age, similar injury forces usually results instead in rupture of the quadriceps tendon above the kneecap.
It is vital that surgery be done early to pull the tendon back to its normal place (with circlage wires) or complications are very likely, and include a high riding kneecap with pain in the front of the knee. Joint cartilage damage may follow. The kneecap may also get stuck down with scar tissue (arthrofibrosis).
Over-enthusiastic repair with insufficient rehab may lead to a low-riding kneecap, patella baja (which is drastic).
Patellar fractures
A patellar fracture is a break of the kneecap bone, usually the result of a hard blow to the front of the knee - falling on the knee, dashboard impact etcetera.
A simple fracture means that the injury does not break through the skin and a compound fracture means that it does. A comminuted fracture means that the bone has splintered in a number of directions, which makes management difficult and the outcome often poor.
In Brief: Patellar Fractures. Scolaro J, Bernstein J and Ahn J. Clin Orthop Relat Res. 2011 Apr; 469(4): 1213–1215.
Current concepts review: Fractures of the patella. Gwinner C, Märdian S, Schwabe P, Schaser K-D, Krapohl BD and Jung TM. GMS Interdiscip Plast Reconstr Surg DGPW. 2016; 5: Doc01.
PREVIOUS PART: Cartilage damage of the patella
END OF PRIMER