Meniscal trimming and meniscal repair are both options to try to avoid a meniscectomy.
 First published in 2011, and reviewed August 2023 by Dr Sheila Strover (Clinical Editor)
First published in 2011, and reviewed August 2023 by Dr Sheila Strover (Clinical Editor)
Not every meniscus tear will come to surgery.
What happens if you leave a torn meniscus untreated?
When knee surgeons decide to tackle a meniscus tear surgically it is because they are trying to prevent instability of the knee which may lead to the forces through the knee not being properly deflected or absorbed by the meniscus, and which can then cause cartilage damage and ultimately arthritis. But not every tear needs immediate surgery, and small tears - especially if longitudinal and near the periphery in the red zone - can just be monitored to see if healing does occur. If a symptomatic meniscus tear is causing ongoing pain, and feelings of instability in the knee, however, it may be that the tear is not healing or is extending, and surgery should be contemplated.
Simple non-symptomatic degenerative tears diagnosed during an unrelated arthroscopy again probably do not need active management - the consensus is that these should simply be left alone.
If an MRI scan done for other reasons suggests a small meniscus tear, but the patient has no symptoms to corroborate this, then one should probably accept this as an error of radiographic interpretation because there are several anatomical structures that seen from certain angles may look like a tear.
Surgical management of degenerative meniscus lesions: the 2016 ESSKA meniscus consensus. Beaufils P, Becker R, Kopf S, Englund M, Verdonk R, Ollivier M and Seil R. Knee Surg Sports Traumatol Arthrosc. 2017; 25(2): 335–346.
Reporting knee meniscal tears: technical aspects, typical pitfalls and how to avoid them. Bolog NV and Andreisek G. Insights Imaging. 2016 Jun; 7(3): 385–398.
What is a meniscal repair?
Knee surgeons these days will generally try to repair a torn meniscus where practical.

meniscal suture
Surgeons often mention that they repaired the meniscus using an 'inside-out' technique. This is a technique where thin tubes (cannulae) with an end like a hypodermic needle are pushed through the skin into the knee joint, and a fine flexible needle pre-threaded with a suture is passed through the cannula and then the one side of the meniscal tear and out through an incision in the skin. The same needed, still with a thread attached, is then passed through the other side of the meniscal tear and again out through the skin incision. Then the cannula and needle are removed, leaving a suture through the two sides of the meniscus, and the loose ends are tied outside of the joint where the incision was made, and the skin is closed over the knot.
Usually the fixation is bio-absorbable, and holds its strength just long enough for healing to occur, before getting absorbed by the body, leaving no sign of the repair material.
meniscal arrows
Meniscal arrows are little half-inch long harpoons, just a millimetre wide, and made of a bio-degradable polyester. They are shot through the two surfaces of the tear to hold the edges together via little barbs. Very occasionally one may work loose and catch in the joint, needing to be removed surgically, but this is very uncommon. The advantage of the arrows over sutures is speed.
suture anchors
Suture anchors may be used in difficult circumstances like root tears. The anchor is inserted into the top of the tibia bone, and it comes pre-loaded with sutures that are then used for the soft-tissue repair.
Arthroscopic Lateral Meniscus Root Repair With Soft Suture Anchor Technique. Prasathaporn N, Kuptniratsaikul S and Kongrukgreatiyos K. Arthrosc Tech. 2013 Nov; 2(4): e479–e482.
T-Fix anchor sutures for arthroscopic meniscal repair. Escalas F, Quadras J, Cáceres E and Benaddi J. Knee Surg Sports Traumatol Arthrosc. 1997;5(2):72-6.
tissue adhesives
Blood clot from the patient may be inserted in the tear before repair as a biological adhesive and healing adjuvant, but there are also commercially available tissue adhesives.
Tissue adhesives for meniscus tear repair: an overview of current advances and prospects for future clinical solutions. Bochyńska AI, Hannink G, Grijpma DW and Buma P. J Mater Sci Mater Med. 2016; 27: 85.
Arthroscopic repair of the meniscus. Vaquero-Picado A and Rodríguez-Merchán EC. EFORT Open Rev. 2018 Nov; 3(11): 584–594.
Rehabilitation following meniscal repair: a systematic review. Spang RC, Nasr MC, Mohamadi A, DeAngelis JP, Nazarian A and Ramappa AJ. BMJ Open Sport & Exercise Medicine 2018;4:e000212. doi: 10.1136/bmjsem-2016-000212.
Thirty years of arthroscopic meniscal suture: What's left to be done? Seil R, VanGiffen N and Pape D. BMJ Open Sport Orthopaedics & Traumatology: Surgery & Research, Volume 95, Issue 8, Supplement, December 2009, Pages 85-96.
What is a meniscectomy?
Modern knee surgeons understand the importance of preserving the meniscus wherever possible, and techniques have been developed to repair tears in the hope of restoring normal anatomy and function. However, certain tears cannot be repaired and it may be necessary for the surgeon to remove meniscal tissue - this is called meniscectomy. In this case the modern surgeon has been taught to preserve as much viable tissue as possible, and especially the all important outer rim.
So the term meniscectomy can encompass different degrees of tissue removal -
partial meniscectomy
The term 'partial meniscectomy' is actually used rather loosely in medical reporting. There may be a wide variation in the actual amount of meniscus removed, from minor trimming of a frayed edge to anything short of removing the rim, which is called a sub-total meniscectomy. It is important to ask your surgeon exactly what was/will be removed, and any video record should be kept for later reference.
total meniscectomy
Removing a complete meniscus, that is a medial or a lateral meniscus, right up to and including the meniscal rim is called total meniscectomy.
Today's focus on meniscal preservation was not always the case, and only two decades ago it was commonplace for surgeons to remove the whole meniscus with little regard for the long term consequences, as the importance of the menisci in load bearing, shock absorption and knee stability had not at that stage been fully appreciated.
MRI Evaluation of Isolated Arthroscopic Partial Meniscectomy Patients at a Minimum Five-Year Follow-up. Williams RJ, Warner KK, Petrigliano FA, Potter HG, Hatch J and Cordasco FA. HSS J. 2007 Feb; 3(1): 35–43.
Total meniscectomy in adolescents: a 40-year follow-up. Pengas IP, Assiotis A, Nash W, Hatcher J, Banks J and McNicholas MJ. J Bone Joint Surg Br. 2012 Dec;94(12):1649-54. doi: 10.1302/0301-620X.94B12.30562. (Erratum in J Bone Joint Surg Br. 2013 Feb;95-B(2):286.)
Medial or lateral meniscectomy?
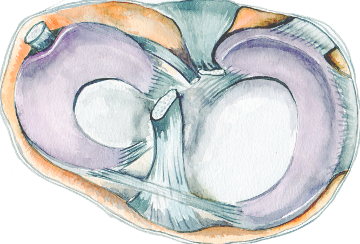 There are a number of important differences anatomically between the medial meniscus (on the inner aspect of the knee) and the lateral menicus (on the outer aspect).
There are a number of important differences anatomically between the medial meniscus (on the inner aspect of the knee) and the lateral menicus (on the outer aspect).
The lateral meniscus in O-shaped. Its outer rim is only loosely attached to the joint capsule, and the meniscus moves freely, its main tethering being to the flattened top of the tibia bone at the anterior and posterior horns. At the back of the lateral meniscus the capsular attachment is completely interrupted by a tendon, called the popliteus tendon. This tendon tensions the lateral meniscus when the knee is bent, and prevents it being crushed by the femur.
Any tear or surgical resection into the rim of the lateral meniscus affects its 'hoop integrity' and there will be a significant disruption of its function.
The medial meniscus is different from the lateral meniscus in several respects. It is larger, and it is C-shaped rather than O-shaped. There is no popliteus tendon interrupting its outer capsular attachment, which is much more evident and stronger than than on the lateral side. All this tethering means that the medical meniscus is less able to move, and is more frequently injured.
Structural and functional consequences of total meniscectomy
Now, there is one big issue about total meniscectomy that you must understand - losing the cushioning rim around the outer edge of the meniscus in a complete meniscectomy is a one-way ticket to arthritis!
Removal of the all-important meniscal rim causes the following consequences -
- shock absorption is lost forever
- since the spacer on the one side of the joint is missing, more forces are transmitted through that side of the joint
- the joint surfaces of the femur (thighbone) and tibia (shinbone) are going to become stressed, softened, and eventually break down ('arthritis') and there will be arthritic pain
- the leg may go on to develop 'bow legged ness' or 'knock-knees', due to the collapse of the joint on the one side (one 'compartment')
- the knee may seem to thrust outwards with each step, further stressing the joint ('lateral thrust')
- the bone may attempt to try to heal the problem - causing totally unhelpful bony outgrowths called 'osteophytes' ('bone mushrooms'). These may form at the joint line or in the notch where the cruciate ligaments reside.
- eventually the cruciate ligaments may become incompetent and rupture
The consequences of meniscectomy. McDermott ID and Amis AA. The Bone & Joint Journal, VOLUME 88-B, ISSUE 12 / DECEMBER 2006.
Long-Term Follow-Up of Open-Meniscectomy: A Case Report and Literature Review. Bell J and Glaser J. Iowa Orthop J. 2001; 21: 73–75.
Monitoring the knee joint after meniscectomy
After a meniscus has been removed the patient may initially notice little alteration in these parameters. Indeed, initially the patient may be delighted at the improvement in their symptoms, but with time negative changes are likely to become apparent.
changes to the joint cartilage in the absence of symptoms
Although the patient who has had a meniscectomy may have none or few symptoms, cartilage-sensitive MRI scans may reveal subtle changes to the joint cartilage1. This may identify the patient at future risk of joint cartilage breakdown and subsequent arthritis.
deterioration in functional knee scores
If taken through a scoring system such as the Knee injury and Osteoarthritis Outcome Score (KOOS), the patient will answer questions that include changes in their activities of daily living and quality of life. Comparison with pre-injury answers and with answers over a period of time after surgery may reveal a gradual deterioration even though the patient may not complain particularly of pain 2.
decreased gap between long bones on stress testing
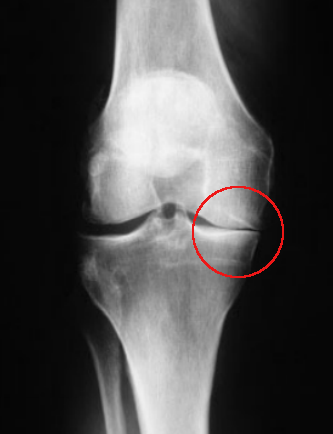
Between the long bones of femur and tibia on X-ray, there is a gap which is the space occupied by the normal meniscus. It shows as a gap because the meniscus is not easily visible on X-ray.
This X-ray actually already shows signs of joint damage, but ignore that for now and just observe the differences in the gap. The red circle shows the gap completely closed - compare the other side which is normal.
Early non-weight-bearing X-rays after a meniscectomy may look completely normal, but taking the X-rays while the joint is being stressed to the side (varus or valgus stress), or while the patient is standing, may demonstrate that the gap is less on the affected side, even though the patient may not be symptomatic.
abnormal sideways thrust during walking
As the stability of the knee becomes stressed by the lack of the meniscus, there may be the development of a sideways thrust of the knee during walking. This happens as the patient shifts their weight onto the meniscectomised knee. The thrust occurs because of the lack of the meniscus which usually is there as a spacer and shock absorber. Depending on the direction of the thrust this is called varus thrust or valgus thrust.
In someone with a thrust like this, the knee might look completely normal to the observer when the patient simply stands still.
abnormal standing leg alignment
In investigations of structural and functional changes like these, it is important to take X-rays with the patient standing and weight bearing. This may reveal alignment problems not evident otherwise, such as a varus deformity (bow leg) rather than the sort of functional thrust seen in the video above.
unicompartmental osteoarthritis
Long term studies of patients after meniscectomy highlight the issue of the development of osteoarthritis2. On X-ray, this may be demonstrated by flattening of femoral condyle (as in the above X-ray), lipping of joint edges and later frank bony outgrowths called osteophytes.
PREVIOUS PART: Meniscal cyst
NEXT PART: Unloading a painful meniscus-deficient knee