Knee surgeon, Angus Strover, offers an overview of things that can be missed during routine diagnostic arthroscopy.
 First published by knee surgeon Angus Strover in 2008, and reviewed August 2023 by Dr Sheila Strover (Clinical Editor)
First published by knee surgeon Angus Strover in 2008, and reviewed August 2023 by Dr Sheila Strover (Clinical Editor)
It is hard for a patient to accept that their diagnosis can be missed due to faulty technique. But it happens a lot with knee surgery.
This is a tragedy for patients, as they may continue struggling with their knee problem until arthritis eventually ensues, rather than having their problem competently dealt with during the first arthroscopic procedure.
In this lesson I am going to list for you some of the common reasons why problems may be missed.
Inadequate visualisation
Missed chondromalacia and missed chondral stripping
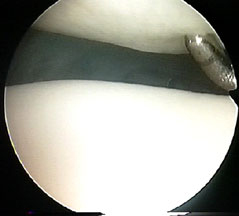
Chondromalacia is not a disease - it is a condition of the hyaline cartilage covering the joint surfaces in the knee, when the cartilage becomes softened. When a knee joint is under stress, the cartilage often goes boggy and is easily dimpled by the examining probe, instead of looking and feeling resilient. In this image the probe easily dents the abnormally soft cartilage.
With time the damaged cartilage, without actually appearing broken, may strip away from the underlying bone and hence its connection to its blood supply.
In both these stages, the cartilage may appear to the eye to be perfectly normal. If the surgeon omits to feel the surface all over carefully with the probe he may miss these important signs.
Missed chondral flap
Once the cartilage has actually torn, a flap of cartilage may occasionally be nipped in the joint - giving symptoms of catching and giving way.
Sometimes the flap may not be evident unless the bony surfaces are carefully and systematically probed.
Failure to locate and deal with such a problem may lead to extension of the defect.
Missed osteochondritis dissecans
This is a disorder, often starting in young people, when the blood supply to a small section of joint cartilage becomes damaged, leading to death of a cone of bone.
Initially the cartilage is intact, and the disorder is suspected on the patient's history and x-rays, but it may be missed if the joint is not adequately and systematically examined as the joint surface may be intact and look normal.
Missed loose body
Failure to examine the lateral gutters or the space behind the cruciate ligaments may mean that a loose body remains undetected.
Even very large loose bodies may be missed. One of the problems is that the fluid flow drives the loose body away from the arthroscope and into one of these deeper situations.
Missed anterior cruciate ligament tear or avulsion
The cruciate ligaments can often look completely normal on initial arthroscopic examination.
Systematic probing and pulling may, however, reveal:
- that a tear is completely concealed by an overlying infrapatellar plica, which may look just like a cruciate ligament
- that the ligament is, indeed intact, but completely incompetent - having pulled away from its bony attachment to either tibia or femur
- that the ligament looks normal, but may be completely ruptured and incompetent - because its casing is intact while the inner fibres have ruptured
- that the posterior cruciate is torn but hidden by the anterior cruciate, unless the ACL is pulled to one side to reveal the PCL behind it
- one or other of the ligaments may have torn and be incompetent, but may look normal - having reattached itself to the other ligament
Missed meniscal tear
A meniscus may often look completely normal in the presence of a tear, as the tear may close up, but not be healed - only to be revealed when the probe enters it.
A meniscus tear may also be horizontal. The top surface of the meniscus may look normal, but careful probing may reveal a deep horizontal tear.
Pulling the edges of an apparently normal meniscus may reveal that the meniscus has 'avulsed' (pulled away) from its bony attachments. This may also occur at the horns.
Missed pathological plica
Failure to examine the knee from above during arthroscopy, and to flex and extend the knee during this part of the procedure, may result in the surgeon missing maltracking, patellar tilt or an abnormal plica. I would advocate that every arthroscopy should include this step.
