The triggering of the arthrofibrosis cascade in the knee after injury or surgery sometimes takes clinicians by surprise.
 First published by Dr Noyes in 2008, and reviewed August 2023 by Dr Sheila Strover (Clinical Editor)
First published by Dr Noyes in 2008, and reviewed August 2023 by Dr Sheila Strover (Clinical Editor)
Arthrofibrosis - course
- Introduction to arthrofibrosis
- The knee - range of motion
- Anatomic classification of arthrofibrosis
- What triggers arthrofibrosis?
- Early signs and symptoms of arthrofibrosis
As arthrofibrosis can be successfully alleviated if treated in its early stages, the clinical team must carefully watch for this complication relatively soon after the initial trauma or surgery, especially if there is an established risk such as in cruciate ligament surgery or arthroplasty.
How does the surgeon or therapist know that the process of arthrofibrosis has been triggered? How can they determine early that a patient's recovery is not progressing normally?
Normal Expectations after Surgery or Injury
We established in Part II the normal range of knee motion in regard to flexion and extension. In the early acute inflammatory phase following injury or surgery, the knee may be painful, swollen, warm, and unable to achieve full motion.
After approximately 2 to 3 weeks, patients should be able to regain normal flexion and extension or demonstrate a normal progression of motion, depending on the operative procedure which was performed. For instance, after high tibial osteotomy we expect patients to be able to achieve 0-110° by the end of the 2nd postoperative week; 0-130° by the end of the 4th week; and full motion by the end of the 6th week.
In patients in whom arthrofibrosis triggers, this 2-week 'turnaround' or normal progression of motion does not occur. In some cases, the knee may do well for the first few weeks following injury or surgery, but then motion becomes limited.
How can the clinician realize that there is an abnormal scarring reaction occurring in the knee?
High Index of Suspicion
The clinician should be alert to the possibility of this complication in disorders in which a higher than normal risk exists - we discussed these disorders in Part IV and briefly in Part I. In 'high-risk' disorders, the patient needs to be managed closely by the surgeon and rehabilitation unit so that healing can be assessed and serial measurements made of knee flexion and extension, the mobility of the patella and its related tendons,and the strength of the quadriceps muscles.
Our research has shown (ref 1) that the progression of arthrofibrosis can trigger downward migration of the patella as early as a few weeks after ACL reconstruction, and crippling patella infera within 8 months to a year. An effective way to monitor this carefully is by the serial measurement of patellar height on a lateral X-ray of both knees.
Two ratios have become standard in the assessment of patellar position - these are the Insall-Salvati and Blackburne-Peel vertical height ratios.
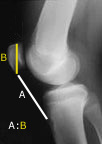
Insall-Salvati ratio - length of the patellar tendon (lowest pole of the patella to the tibial tubercle on X-ray) compared to the height of the patella - usually 1.02 +/- 0.2. A ratio of less than 0.8 is considered to be patella infera.

Blackburne-Peel ratio - lowest point on the patellar cartilage to the level of the tibial plateau compared to the length of the patellar articular surface - usually 0.54-1.06. A ratio of less than 0.54 is considered to be patella infera.
In 1991, (ref 2) two colleagues and I compared the two knees of 51 individuals and found that, although the ratio may vary slightly from person to person, it is remarkably consistent between the two knees of the same person. This allowed us to diagnose patella infera by comparing the ratio in the problem knee with that in the normal knee on serial lateral X-rays with the knee in 30-60° of flexion.
Caveat - Remember that a limitation of ROM may have causes other than arthrofibrosis
In the investigation of a patient's lack of progress, the careful clinician must exclude other mechanical causes for the joint stiffness -
- muscle inhibition
- fluid in the joint (including infection)
- mechanical factors, such as a loose body, bucket-handle tear of the meniscus, or cyclops lesion
- joint bones out of alignment, eg from a fracture (break)
- interruption to the extensor mechanism, eg ruptured patellar tendon
- improperly placed ligament graft
- damaged nerves
These conditions may trigger or be present in combination with arthrofibrosis.
References
1. Noyes FR, Mangine RE, Barber S. Early knee motion after open and arthroscopic anterior cruciate ligament reconstruction. Am J Sport Med. 1987;15:149-60.
2. Noyes FR, Wojtys EM, Marshall MT. The early diagnosis and treatment of developmental patella infera syndrome. Clin Orthop. 1991;265:241-52.
PREVIOUS PART: What triggers arthrofibrosis?
NEXT PART: Established arthrofibrosis - options for management
