 Baker's Cyst has nothing to do with baking!
Baker's Cyst has nothing to do with baking!
The condition is named after the doctor who first formally described it - William Morrant Baker (1838–1896), an English anatomist and surgeon who described a cystic swelling at the back of the knee.
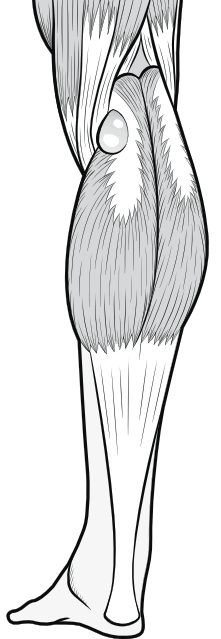
The region at the back of the knee is called the popliteal region, and the diamond-shaped recess in the middle of it is called the 'popliteal fossa'. Pain experienced in this region is very common, but it may be a bit of a challenge to the doctor to determine what is causing it. The most common cause is a Baker's cyst (popliteal cyst). A cyst is an abnormal pocket of fluid, usually closed off, but a Baker's cyst communicates with the cavity of the joint. When fluid builds up in the joint cavity, it exerts pressure on the waterproof walls of the capsule, but in the popliteal region there is a weakness in the capsule (at an area known as the gastrocnemius-semimembranous bursa) and the wall bulges out.
What causes a Baker's Cyst?
A misconception is that it is the cyst that is the basic abnormality, but in fact the question that needs to be asked is 'why is the joint fluid building up so much that it pushes out through this weak area?'
A small amount of joint fluid is normal. The inner lining of the joint capsule secretes this fluid and it nourishes the cartilage covering the ends of the bones of the joint. If there is any abnormality inside the knee, such as arthritis or a torn meniscus (especially a torn posterior horn), then the lining responds by increasing the production of this joint fluid. So a Baker's cyst may be an expression of something else going on inside the knee, and the doctor will need to investigate to determine the underlying problem. Where there is a physical connection between the joint cavity and the cyst, resolution of the underlying problem generally leads to a resolution of the cyst. However, occasionally the neck of the cyst pinches off, and the cyst continues to exist without a connection to the joint cavity.
Baker's Cyst Treatment
If the problem does not resolve even after attention to the underlying problem, the patient may be brought in for ultrasound-guided aspiration of the cyst under sterile conditions, and some steroid might be injected in an attempt to reduce inflammation in the area. The patient is likely to be prescribed a period of rest with the leg elevated. The patient should avoid activities like squatting, kneeling and heavy lifting, which aggravate the pain. Hamstrings stretches may help to alleviate the forces through the back of the knee.
Prolotherapy has also been advocated to inflame and scar up the cyst, preventing it completely from filling up again. This is not a mainstream management, because surgeons remain sceptical of prolotherapy, but it may be worth considering.
Surgery is only indicated when other measures have failed.
The modern way of dealing with a troublesome cyst is arthroscopic decompression. The surgeon passes an arthroscope into the knee cavity and enlarges the 'valve-like' part of the capsule at the inside entrance of the cyst, allowing the fluid to pass back into the knee cavity rather than having pressure maintained in the cyst. This method is preferable to that of draining the cyst from the back of the knee, because there are vascular structures that could become damaged, and the root cause of the problem is not properly addressed.
CLINICAL PUBLICATIONS
Arthroscopic internal drainage and cystectomy of popliteal cyst in knee osteoarthritis Jiang J and Ni L. J Orthop Surg Res. 2017; 12: 182.
Baker’s Cyst - Diagnostic and Surgical Considerations Frush TJ and Noyes FR.Sports Health. 2015 Jul; 7(4): 359–365.
Baker's Cyst - Everything You Need To Know - Dr. Nabil Ebraheim via the University of Toledo Foundation Department of Orthopaedic Surgery
